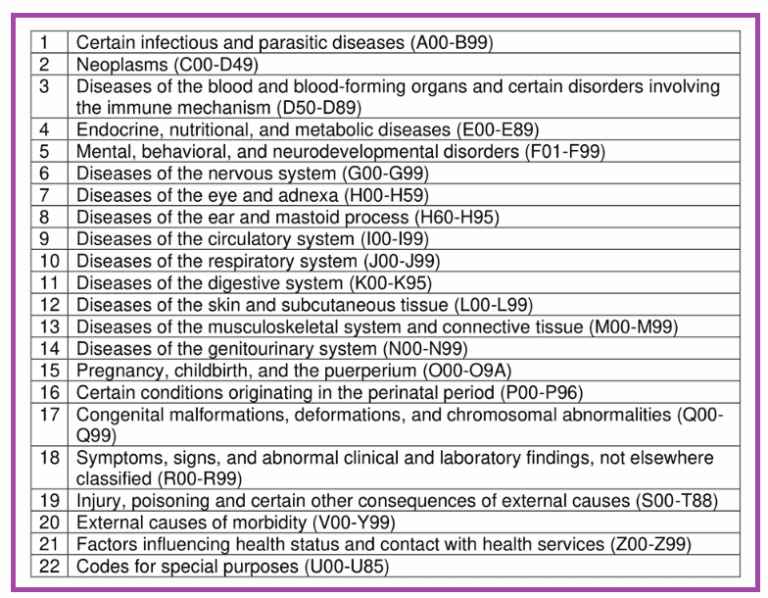
Patient and hospital-level variables provided by HCUP NRD were used to identify demographics and baseline characteristics. We identified our cohort using the ICD-10 codes for OA and RA used for inpatient PCI for the years 20 (Table S1). The codes used are summarized in Table S1. We identified our cohort, procedures, and outcomes using the International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) and Procedure Coding System (ICD-10-PCS) codes along with ICD-10 Clinical Classifications Software (CCS). The NRD contains discharge data from 28 geographically dispersed states, accounting for 60.0% of the total US resident population and 58.2% of all US hospitalizations. We used the Nationwide Readmissions Database (NRD) of the Healthcare Cost and Utilization Project (HCUP), Agency for Healthcare Research and Quality, to obtain our cohort. We performed a comprehensive analysis of the Nationwide Readmissions Database (NRD) to describe the outcomes of RA and OA. Both modalities help enlarge the lumen and enhance equipment delivery. It uses a drive shaft with an eccentrically mounted crown to perform proximal and distal sanding that is abrasive only to fibrotic and calcified vessels, minimizing damage to the medial layer of the vessel. Paul, MN, USA) was approved in 2013 as an adjunctive tool for PCI in heavily calcified vessels. Orbital atherectomy (OA) (Cardiovascular Systems, Inc., St. RA uses a rotating abrasive burr at high speeds to ablate and crack superficial calcium. Rotational atherectomy (RA) (Boston Scientific, Natick, MA, USA) has been the traditional modality for treating calcified coronary lesions in the United States for the past three decades. The main contemporary indication of atherectomy devices is the preparation of the vessel for subsequent balloon angioplasty and stenting. Different calcium-specific technologies are available to address coronary calcification, including atherectomy devices and, more recently, intravascular lithotripsy, which is yet to be approved for coronary use in the United States. The prevalence of moderate to severe calcification in patients undergoing PCI is around 20% angiographically. Severe coronary artery calcification is a significant risk factor for procedural failure and complications, and long-term adverse events in contemporary percutaneous coronary intervention (PCI). OA was noted to have a lower incidence of in-hospital death, but a higher risk of coronary perforation and a higher cost of index hospitalization for the overall unmatched cohorts. There was no change in the trend of use for either modality over the years 20. RA remains the predominant atherectomy modality for inpatient PCI in the United States (93%). 0.2%, p = 0.009), but a higher risk of coronary perforation (1.7% vs. In our cohort, OA was associated with lower in-hospital mortality (3.1% vs. 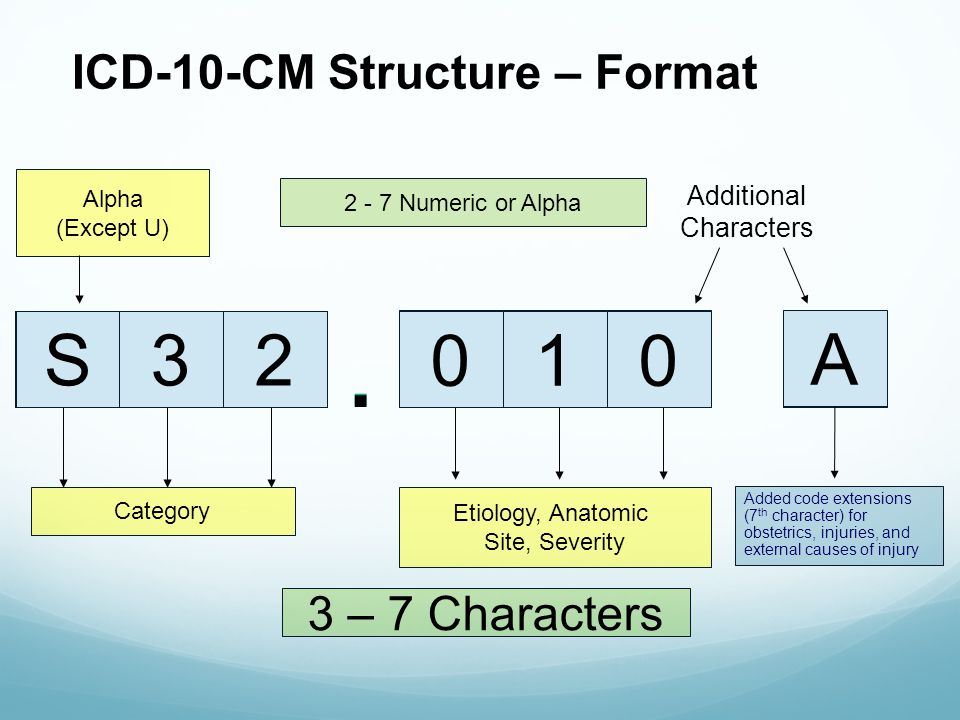
OA was less utilized in patients presenting with ST-segment elevation myocardial infarction (STEMI) (4.3% vs. There was no significant change in the trend of using OA or RA over 20. We included 77,040 records of patients who underwent inpatient PCI with atherectomy. We conducted a multivariate regression analysis to identify variables associated with in-hospital mortality. We queried the Nationwide Readmission Database (NRD) from January to November for the years 2016–2017 to identify hospitalizations of patients who underwent PCI with atherectomy. RA in contemporary inpatient PCI are limited. rotational atherectomy (RA) use for inpatient percutaneous coronary intervention (PCI) in the United States. Our objective was to describe the contemporary outcomes of orbital atherectomy (OA) vs.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
